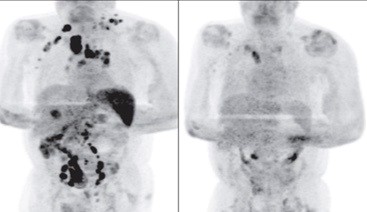
A 61‐year‐old man with stage III Hodgkin lymphoma was hospitalized for the infection of Covid-19 in the UK. He was hospitalized for 11 days and did not receive any cancer treatment. Four months later, the PET-CT scan result showed that his lymphoma was largely gone!
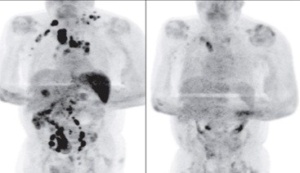
Left: Before, Right: After
Everyone were suppressed, including his doctors and the scientists who saw the results, and no one knows what has caused the cancer remission if no anticancer drugs have been given during the course of his disease.
After looking at a similar case in the US, doctors and scientists have concluded that the most probable reason of his remission is the combined actions of his immune system: for unknown reasons, the patient’s own immune system was activated by the Covid-19 infection, and the anticancer power of T-cells and natural killer cells was released. Together with their anti-viral functions, they attacked both Covid-19 infected cells and the lymphoma cells.
Although this news is very exciting, it’s the only report so far regarding Covid-19 induced cancer remission. The chance of making the Covid-19 infection an anticancer therapy is extremely low as it’s dangerous and even life-threatening to most cancer patients. But what this rare case shows us is a future with hopes: the immuno-oncology drugs and immunotherapies currently under development may actually cure certain types of cancer in the near future.
Cancer vaccine-based therapy is one of the options among those emerging immunotherapies. Using genetic engineering technology, scientists could identify unique neoantigens, a type of cancer specific molecules, and then create vaccines that enable the key immune cells, including T-cells, to recognize and kill those cells that carry the neoantigens. Just like what the virus infection did to the cancer patient, after the cancer vaccine is administered, the patient’s own immune system will be activated and the T-cells and other immune cells will be taught and directed to recognize and destroy the cancer cells.
Several cancer vaccines are currently being tested in clinical trials to see if the combination of cancer vaccines with immune-oncology drugs will bring better treatment effects than using the them alone.
New drugs bring new hope. Ask your doctor about the cancer vaccine related therapies and find out if you could benefit from them.
References
SARS‐CoV‐2‐induced remission of Hodgkin lymphoma. British Journal of Haematology; January2, 2021. https://doi.org/10.1111/bjh.17116
Complete spontaneous remission of diffuse large B-cell lymphoma of the maxillary sinus after concurrent infections. Clinical Lymphoma, Myeloma & Leukemia; 2012; 12:455– 8. https://pubmed.ncbi.nlm.nih.gov/23025990/
Individualized neoantigen vaccines. Nature Research; September 28, 2020. https://www.nature.com/articles/d42859-020-00026-3
Personalized cancer vaccine clinical trial to expand following promising early results. University of Arizona Health Sciences; November 10, 2020. https://www.sciencedaily.com/releases/2020/11/201110102550.htm